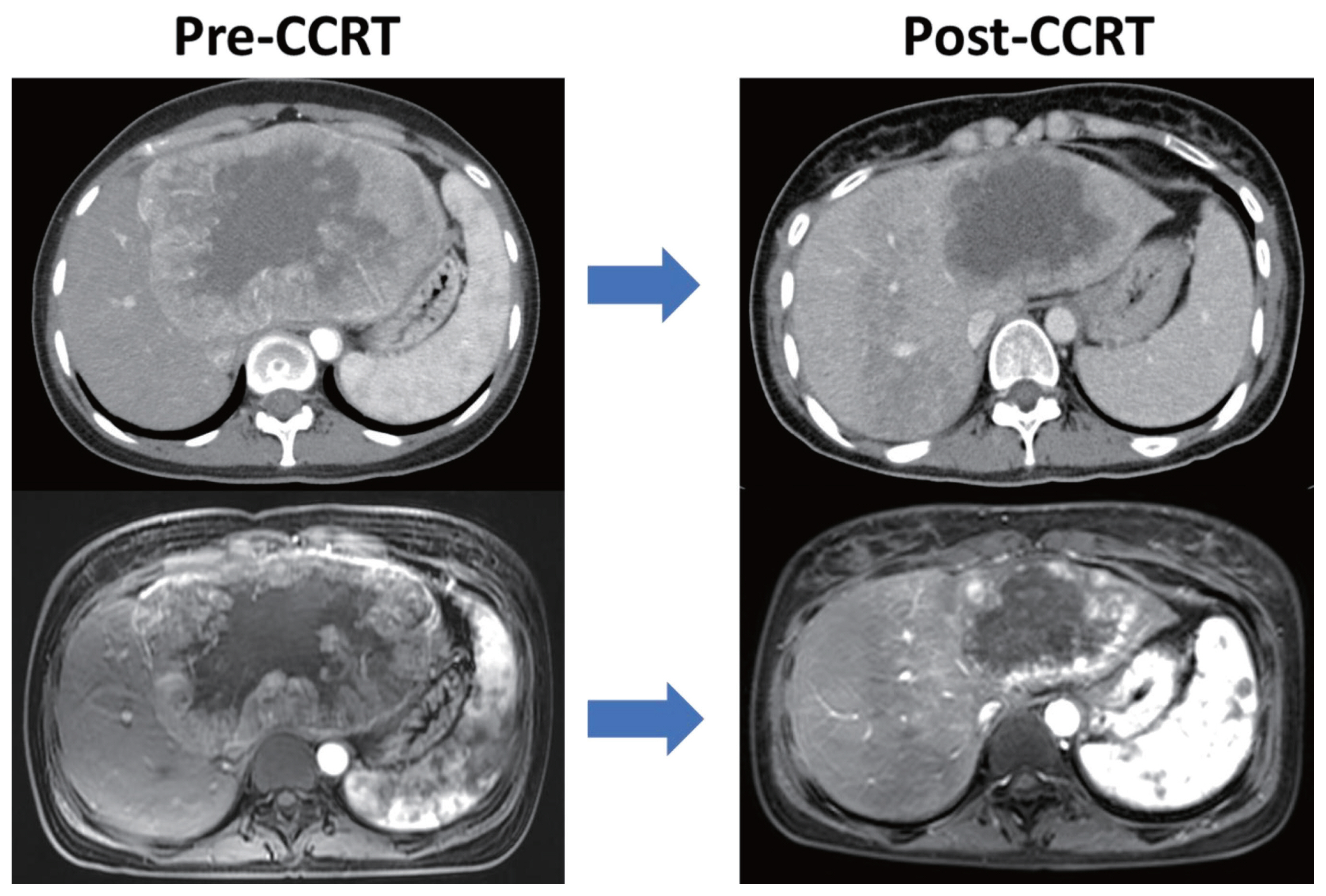
- Favorable response of hepatocellular carcinoma with portal vein tumor thrombosis after radiotherapy combined with atezolizumab plus bevacizumab
-
Yong Tae Kim, Jina Kim, Jinsil Seong
-
J Liver Cancer. 2023;23(1):225-229. Published online March 16, 2023
-
DOI: https://doi.org/10.17998/jlc.2023.02.27
-
-
1,080
Views
-
69
Downloads
-
2
Citations
-
 Abstract Abstract
 PDF PDF
- Recently, the superiority of atezolizumab plus bevacizumab (AteBeva) over sorafenib was proven in the IMbrave150 trial, and AteBeva became the first-line systemic treatment for untreated, unresectable hepatocellular carcinoma (HCC). While the results are encouraging, more than half of patients with advanced HCC are still being treated in a palliative setting. Radiotherapy (RT) is known to induce immunogenic effects that may enhance the therapeutic efficacy of immune checkpoint inhibitors. Herein, we report the case of a patient with advanced HCC with massive portal vein tumor thrombosis treated with a combination of RT and AteBeva, who showed near complete response in tumor thrombosis and favorable response to HCC. Although this is a rare case, it shows the importance of reducing the tumor burden via RT to combination immunotherapy in patients with advanced HCC.
-
Citations
Citations to this article as recorded by  - Feasibility of additional radiotherapy in patients with advanced hepatocellular carcinoma treated with atezolizumab plus bevacizumab
Tae Hyun Kim, Bo Hyun Kim, Yu Ri Cho, Young-Hwan Koh, Joong-Won Park
Journal of Liver Cancer.2023; 23(2): 330. CrossRef - Carbon Ion Radiotherapy in the Treatment of Hepatocellular Carcinoma
Hwa Kyung Byun, Changhwan Kim, Jinsil Seong
Clinical and Molecular Hepatology.2023; 29(4): 945. CrossRef
- Long-term survival after multimodal treatment involving radiotherapy for huge hepatocellular carcinoma with oligometastasis: a case report
-
Byung Min Lee, Jinsil Seong
-
J Liver Cancer. 2021;21(2):163-168. Published online September 2, 2021
-
DOI: https://doi.org/10.17998/jlc.2021.08.06
-
-
 Abstract Abstract
 PDF PDF
- The clinical efficacy of local ablative treatment for oligometastasis is widely accepted in most cancers. However, due to limited data, this has not been the case for hepatocellular carcinoma (HCC). Here, we report a case of pulmonary oligometastasis of a huge HCC that was treated by multimodality with liver-directed concurrent chemoradiotherapy (CCRT) plus subsequent resection of the primary lesion and local ablative radiotherapy (RT) for subsequent lung oligometastatic lesions. In this patient, liver-directed CCRT induced significant tumor shrinkage with compensatory hypertrophy of the non-tumor liver, followed by curative resection. Surgical resection of the first and second pulmonary metastatic lesions as well as local ablative RT of the third lesion achieved complete tumor regression, which led to long-term survival of 6 years. Therefore, the active use of local ablative RT requires full consideration in cases of oligometastatic HCC.
- Curative liver transplantation after lung resection for advanced hepatocellular carcinoma with lung metastasis and inferior vena cava tumor thrombosis: a case report
-
Dong Jin Joo, Do Young Kim, Jinsil Seong, Hyun Jeong Kim, Jae Geun Lee, Dai Hoon Han, Gi Hong Choi, Myoung Soo Kim, Jin Sub Choi, Soon Il Kim
-
J Liver Cancer. 2021;21(2):181-186. Published online September 30, 2021
-
DOI: https://doi.org/10.17998/jlc.2021.09.08
-
-
3,639
Views
-
92
Downloads
-
1
Citation
-
 Abstract Abstract
 PDF PDF
- Hepatocellular carcinoma (HCC) with distant metastasis is an absolute contraindication for liver transplantation (LT). However, it is still unclear whether LT is feasible or acceptable in such patients, albeit after being treated with a multidisciplinary approach and after any metastatic lesion is ruled out. We report one such successful treatment with living donor LT (LDLT) after completely controlling far-advanced HCC with inferior vena cava tumor thrombosis and multiple lung metastases. The patient has been doing well without HCC recurrence for eight years since LDLT. The current patient could be an anecdotal case, but provides a case for expanding LDLT indications in the context of advanced HCC and suchlike.
-
Citations
Citations to this article as recorded by  - Inferior Vena Cava Thrombectomy and Stenting as Bridge to Liver Transplantation After Radiotherapy-Induced Thrombosis
Raphael PH Meier, Shani Kamberi, Josue Alvarez-Casas, Barton F. Lane, Chandra S. Bhati, Saad Malik, William Twaddell, Kirti Shetty, Adam Fang, Hyun S. Kim, Daniel G. Maluf
Progress in Transplantation.2023;[Epub] CrossRef
- Selection of Proper Modality in Stereotactic Body Radiation Therapy for Hepatocellular Carcinoma
-
Seo hee Choi, Joong Yeol Woo, Jinsil Seong
-
J Liver Cancer. 2017;17(1):45-53. Published online March 31, 2017
-
DOI: https://doi.org/10.17998/jlc.17.1.45
-
-
2,424
Views
-
42
Downloads
-
1
Citation
-
 Abstract Abstract
 PDF PDF
- Background/Aim
s: As the optimal stereotactic body radiation therapy (SBRT) modality
for hepatocellular carcinoma (HCC) has not been confirmed, we aimed herein to provide a
practical guideline by our retrospective review.
Methods
Thirty-nine patients with primary HCC who underwent liver SBRT via 3 modalities
(helical tomotherapy [HT]: 22, volumetric modulated arc therapy [VMAT]: 13, Cyberknife: 4)
at our institution between July 2014 and July 2015 were included. Modalities were compared
with regard to dose conformity index (CI), homogeneity index (HI), clinical results, and patient
compliance.
Results
VMAT SBRT had favorable conformity (CI: 0.7±0.2), homogeneity (HI: 1.1±0.0), and
shortest treatment time (100.2±26.1 seconds). HT SBRT yielded good dosimetric outcomes,
especially in conformity (CI: 1.0±0.2). Although the Cyberknife SBRT synchrony system allowed
real-time tumor targeting, the treatment time was longest (3,015.0±447.3 seconds), invasive
pre-treatment procedures were required, and the HI (1.3±0.0) was lowest.
Conclusions
All 3 modalities yielded competent dosimetric planning parameters. VMAT
SBRT was most appropriate for tumors with residual lipiodol or patients with poor conditions.
HT SBRT is available for multiple or irregular targets. Cyberknife SBRT is recommended for
carefully selected patients and tumors indicated for sono-guided fiducial insertion.
-
Citations
Citations to this article as recorded by  - Plan quality analysis of stereotactic ablative body radiotherapy treatment planning in liver tumor
Anirut Watcharawipha, Somvilai Chakrabandhu, Anupong Kongsa, Damrongsak Tippanya, Imjai Chitapanarux
Journal of Applied Clinical Medical Physics.2023;[Epub] CrossRef
- A Case of Partial Response of Hepatocellular Carcinoma Induced by Concurrent Chemoradiation and Hepatic Arterial Infusion Chemotherapy after Trans-Arterial Chemoembolization
-
Myung Eun Song, Sangheun Lee, Mi Na Kim, Dong-Jun Lee, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Sang Hoon Ahn, Chae Yoon Chon, Kwang-Hyub Han, Jinsil Seong, Do Young Kim
-
Journal of the Korean Liver Cancer Study Group. 2013;13(2):152-157. Published online September 30, 2013
-
DOI: https://doi.org/10.17998/jlc.13.2.152
-
-
 Abstract Abstract
 PDF PDF
- A 63-year-old man patient was referred for treatment of infiltrative hepatocellular carcinoma with hilar invasion after transarterial chemoembolization. Serum alkaline phosphatase and bilirubin were elevated, liver dynamic CT showed infiltrative type mass in left hepatic lobe and right hepatic dome with hilar invasion and left intrahepatic duct dilatation. Also CT showed obliteration of left portal vein and metastasis of lymph node around common bile duct. He was diagnosed as hepatocellular carcinoma (UICC stage IV-A, BCLC stage C). With the percutaneous transhepatic biliary drainage and the concurrent chemoradiation therapy and the 4th cycle of hepatic arterial infusion chemotherapy for infiltrative mass, viable tumor was decreased in resectable size at eight months from initial diagnosis.
- High Precision Radiotherapy of Hepatocellular Carcinoma
-
Jinsil Seong
-
Journal of the Korean Liver Cancer Study Group. 2005;5(1):1-6. Published online June 30, 2005
-
-
-
 PDF PDF
|